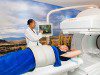
New mobile healthcare solutions from RMI and Acacium Group will combine logistics, staffing, data, and clinical expertise to provide healthcare services at the point of need, no matter where.
The NHS is facing an unprecedented challenge: how to cope with the growing demand for healthcare services, especially in the wake of the COVID-19 pandemic.
According to the latest figures from NHS England, there were 5.6 million people waiting to start treatment at the end of July 2021, the highest number since records began in 2007. Of these, more than 300,000 had been waiting for more than a year, compared to just 1,600 in February 2020.
The impact of this backlog is not only felt by patients, who may suffer from worsening health conditions, reduced quality of life and increased anxiety, but also by healthcare staff, who face increased workload, stress, and burnout. The situation is also likely to worsen as the winter season approaches, bringing with it more pressure on the NHS from flu, colds, and other respiratory infections.
“The mobile clinical model has been proven to reduce pressure on local health services”
Ash Thornley-Davis, Account Executive, Healthcare and the NHS, Zoom


NOT A NEW CONCEPT
To address this challenge, the NHS needs to find innovative and flexible ways to deliver healthcare services that can meet the needs of patients and staff, while also ensuring quality, safety, and efficiency. One such solution is the use of mobile healthcare units, which can provide a range of services in different settings and locations, from diagnostics and testing to treatment and vaccination.
Mobile healthcare units are not a new concept, as they have been used for decades to provide services such as breast screening, blood donation, and dental care. However, advances in technology, logistics, and clinical expertise have enabled the development of more sophisticated and versatile mobile solutions that can offer a wider range of services and specialties.
For example, mobile units can now be equipped with state of the art equipment such as CT scanners, MRI machines, X-ray machines, and ultrasound machines, as well as digital platforms that enable remote consultation, monitoring, and data analysis. Mobile units can also be staffed by qualified and experienced healthcare professionals who can deliver high-quality care in a safe and comfortable environment.
The benefits of mobile healthcare units are manifold. They can increase access to healthcare services for patients who live in remote or deprived areas, or who face barriers such as transport, mobility or language; they can reduce waiting times and pressure on local health services by providing additional capacity and flexibility; they can improve patient satisfaction and engagement by offering more choice and convenience; they can support public health initiatives such as mass testing and vaccination programmes; and they can enhance clinical outcomes by enabling early diagnosis and intervention.
LANDMARK PARTNERSHIP
A recent example of the successful use of mobile healthcare units is the partnership between Acacium Group and RMI Global Solutions (RMI), two expert providers in the global healthcare sector. Acacium Group is the UK’s largest healthcare delivery partner, deploying over 30,000 healthcare professionals a week globally. RMI delivers technical, medical, and security solutions to companies and governments around the world.
“The mobile clinical model has been proven to reduce pressure on local health services, cut down NHS waiting lists, and improve engagement with healthcare services from remote and disengaged communities. Our partnership with Acacium Group is centred on one aim: how we can offer the public and independent sectors healthcare solutions at the point of need, no matter where that is,” says RMI’s UK Managing Director, Julian Rawles.
“RMI’s experience in delivering healthcare in complex and remote environments, partnered with Acacium Group’s capabilities in healthcare workforce deployment and delivery, is unmatched.”
Together, they have launched a new offering that combines logistics, staffing, data, and clinical expertise. The mobile healthcare solutions offering can support with hospital backlogs, accident and emergency (A&E) waiting times, general practice (GP) capacity, school immunisation drives, and even mobile physiotherapy units for occupational health needs.
ABOUT RMI
RMI delivers technical, medical, and security solutions to companies and governments around the world. The company has offices in the Americas, the UK, and Africa, and has been recognised six times by Inc. 5000 as one of the fastest-growing companies in the US. RMI works with Fortune 100 corporations and governments. https://rmiglobalsolutions.com/about-us/
HISTORIC SUCCESS BODES WELL
The partnership has a proven track record of delivering tremendous results, following an award-winning project delivered by RMI and Espirita, part of Acacium Group, on behalf of the Department of Health and Social Care (DHSC). In 2021, in the midst of the COVID-19 pandemic, RMI and Acacium Group established a project team that delivered state of the art mobile testing laboratories manned by 80 logistical and support staff and over 155 scientific and non-scientific staff, within a period of just eight weeks. Clinical staff worked 135,440 hours throughout the course of the project and processed 110,409 samples at key events and during operational exercises. From these, 32,956 positive cases were identified, safeguarding the continued operation of key infrastructure organisations and government functions during the pandemic.
“We deploy over 30,000 healthcare professionals globally every week – our expertise in flexible staffing solutions has shown us how crucial it is to have a highly trained workforce who can be deployed to meet surges in demand. With pressure on healthcare providers seen across the system, having access to a service that is agile and capable of delivering expert healthcare solutions at scale is unique, and has the potential to change the way healthcare challenges are met,” adds Mike Barnard, CEO of Acacium Group.
ABOUT ACACIUM GROUP
Acacium Group is a leading global healthcare delivery partner. With over 35 years of experience and 24 specialist businesses, the group improves people’s lives through expert healthcare, social care, and life sciences. By combining access to workforce, technology, and sector expertise, Acacium Group increases the sustainability of the global healthcare system, from early-stage clinical research right through to palliative care.
Another example of the potential of mobile healthcare units is the virtual ward model, which enables patients to be monitored remotely at home or in the community, using digital devices that transmit vital signs and other clinical data to a central hub, where clinicians can review them and intervene if necessary. This model can reduce hospital admissions and the length of stay, as well as improve the patient experience and quality of care. The King’s Fund, a leading think tank on health and social care policy, has highlighted some successful examples of virtual wards in action, such as those implemented by the Hampshire Hospitals NHS Foundation Trust, North West London Clinical Commissioning Group, and Surrey Heartlands Health and Care Partnership.
The use of mobile healthcare units is not without challenges, however. Some of the barriers that may limit their adoption and effectiveness include the availability and cost of suitable vehicles, equipment and staff; the regulatory and governance frameworks that apply to different services and settings; the integration and interoperability of data and IT systems; the engagement and collaboration of stakeholders, such as commissioners, providers, patients, and communities; and the evaluation and evidence of impact and value.
These challenges can be overcome by adopting a strategic and collaborative approach that involves co-designing, co-delivering, and co-evaluating mobile healthcare solutions with all relevant parties, as well as sharing best practices and learning from other examples. The NHS Long Term Plan, published in 2019, recognised the need for more integrated and community-based care, as well as the role of technology and innovation in transforming health and care services.
Mobile healthcare units can be seen as a key enabler of this vision, as they offer a new way to tackle the NHS waiting list crisis and improve the health and well-being of the population.